Abbott Connect
Every day, medical assistants in small clinics run a point-of-care test, wait for the result, then manually type it into their EHR, one value at a time. A single transposition error can change a diagnosis. Across 220,000+ physician office labs, this isn't a workflow problem. It's a patient safety problem.
Abbott Connect is a cloud-native platform designed to close that gap by connecting point-of-care devices to hospital systems with zero manual transcription, automated compliance, and no infrastructure required.
What we heard
These aren't edge cases. They represent a $7.6–19.7B ambulatory market with zero purpose-built connectivity solutions. That's 220,000+ labs still running on paper binders and manual transcription.
Goals
- Design a cloud-native POC platform that practice managers can set up themselves. No servers, no IT, no professional services. Self-service onboarding in under 2 minutes per device.
- Automate the full CLIA compliance workflow with digital QC logs, operator certification tracking, and one-click audit reports, eliminating paper binders and quarterly site visits.
Competitive Analysis, RALS, AegisPOC, and RelayMed
Abbott Connect complements RALS and AegisPOC by covering a market segment neither was designed to serve.
Competitive positioning: Abbott Connect occupies the high-value quadrant with full platform capability and consumer-grade simplicity
RelayMed ships unconfigured with no compliance or intelligence layer. RALS requires dedicated server infrastructure. Abbott Connect bridges the gap.
Guiding our design direction
Exploring three directions
Three approaches were explored: from familiar healthcare patterns to a significant departure with ambient intelligence.
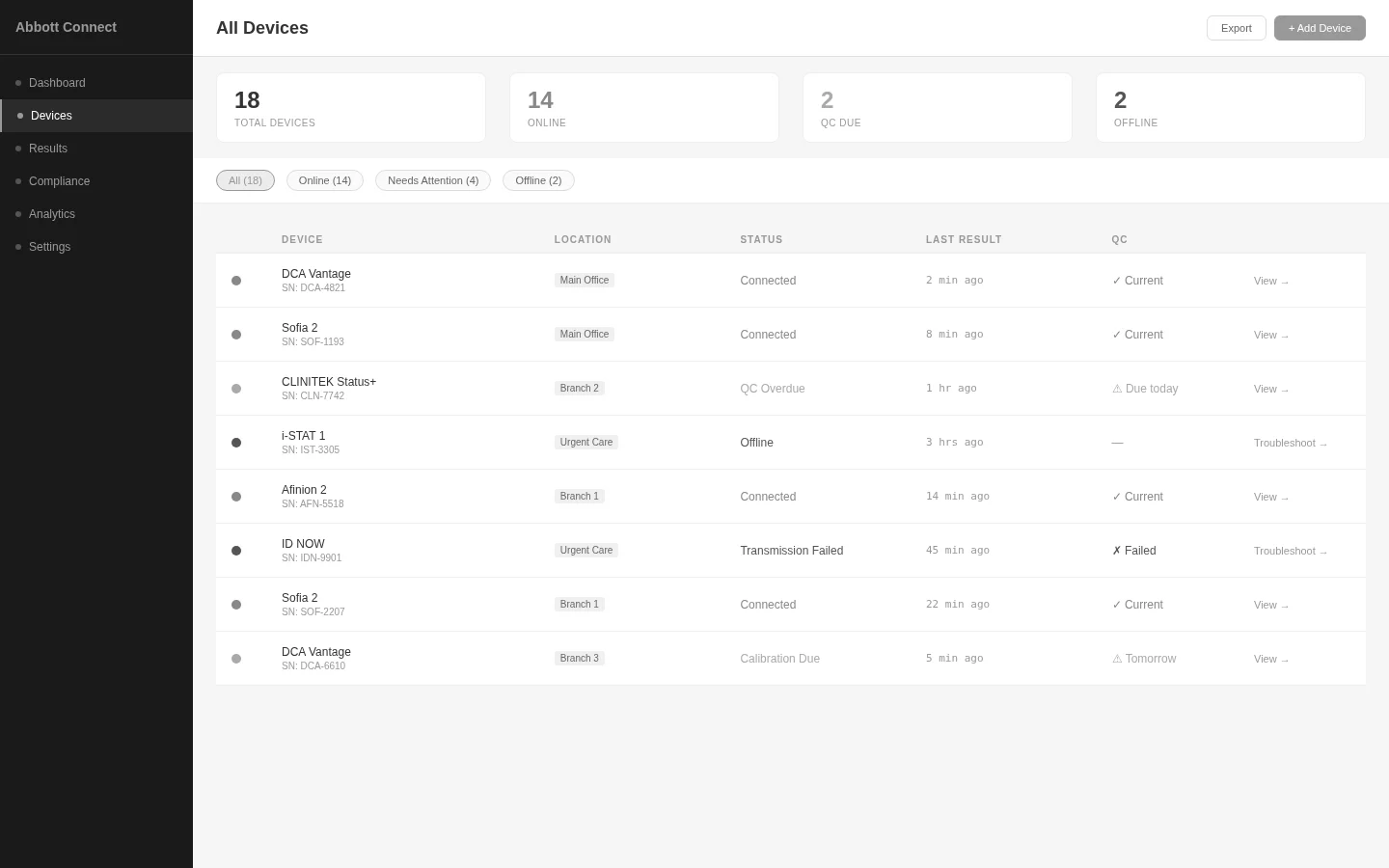
Traditional Dashboard
ExploredGrid view with status indicators. Users manually scan to find issues. Familiar healthcare pattern.
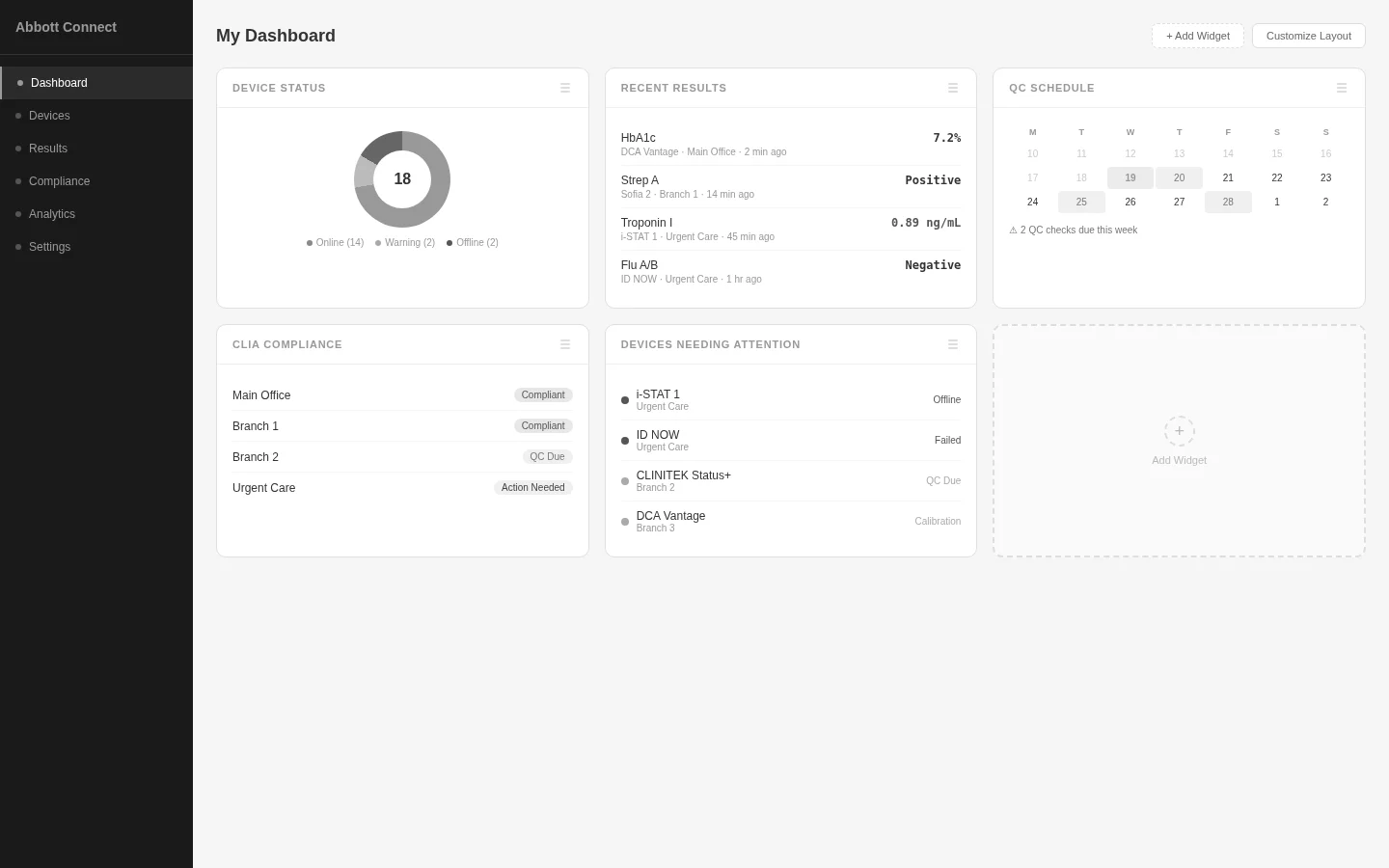
Modular Widgets
ExploredDrag-and-drop widgets for device status, results, and compliance. Similar to Salesforce customization.
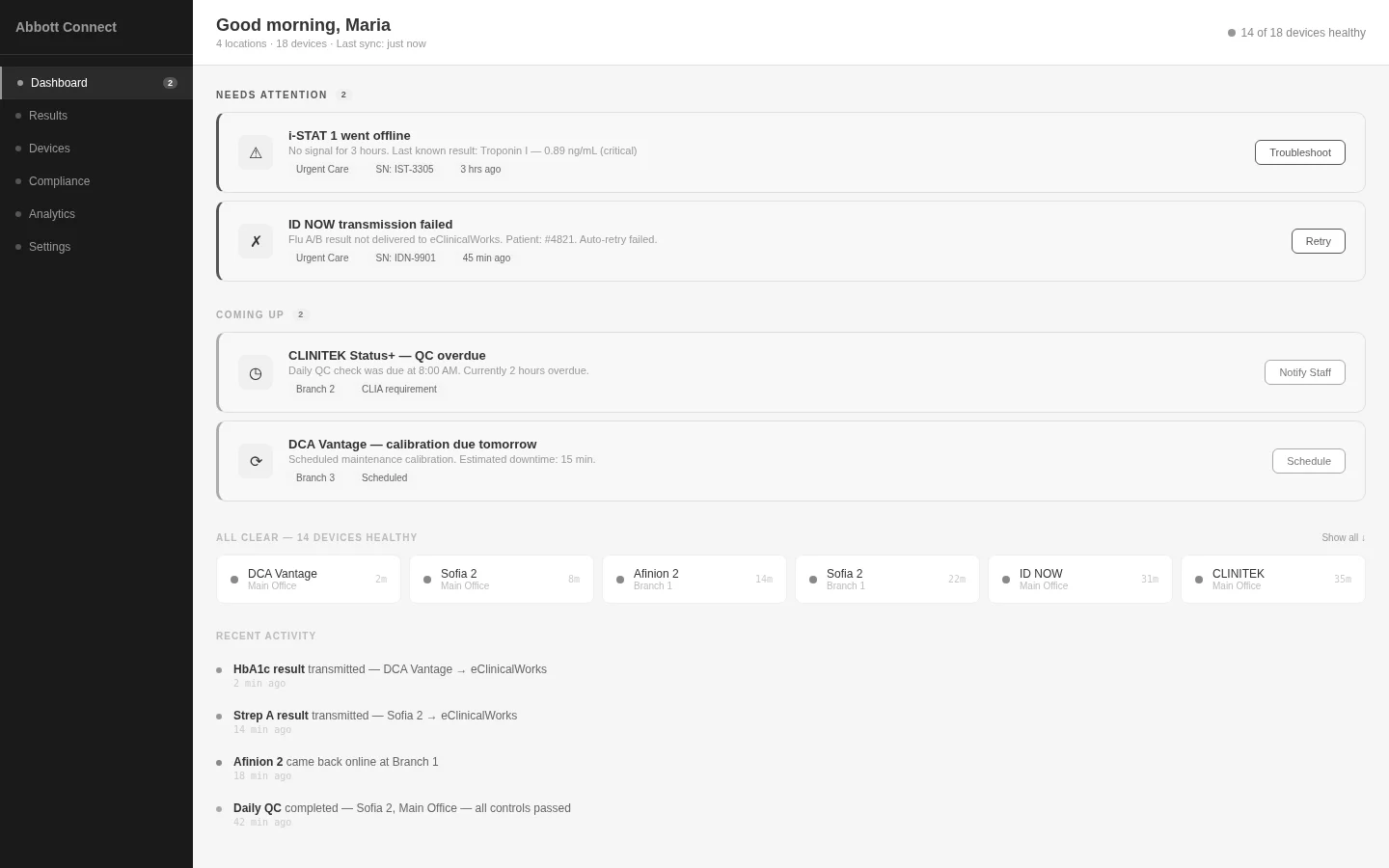
Ambient Intelligence
ShippedSurfaces only what needs attention. Failed devices get alert cards, healthy devices stay quiet. Organized by priority.
How we tested and iterated
Three rounds of testing with lab directors, IT admins, and compliance officers before committing to engineering.
Key iteration from testing: Round 2 revealed that IT admins wanted confirmation at each onboarding step before moving forward, reducing setup anxiety. This led to Design Decision #2, the step-by-step validation flow. Without testing, we would have shipped a continuous form.
Key decisions that shaped the experience
Ambient Dashboard with Contextual Alerts
The dashboard surfaces only what needs attention—failed transmissions, offline devices, upcoming QC. Everything is fine until it isn't.
Six-Step Guided Onboarding Wizard
Six-step progressive wizard: auto-detect devices, validate connectivity, confirm EHR integration, run QC baseline, register compliance, go live.
Result: Setup time dropped from 4+ hours to 28 minutes, an 87% reduction validated across 3 rounds of testing with IT admins.
Real-Time Result Stream with Clinical Context
Auto-transmission to EHR with clinical context (test value, reference range, device source, patient ID) in under 60 seconds, not 8 minutes.
Before Abbott Connect, manual transcription introduced a 3.7% error rate across point-of-care results. With automated EHR transmission, that number drops to zero.
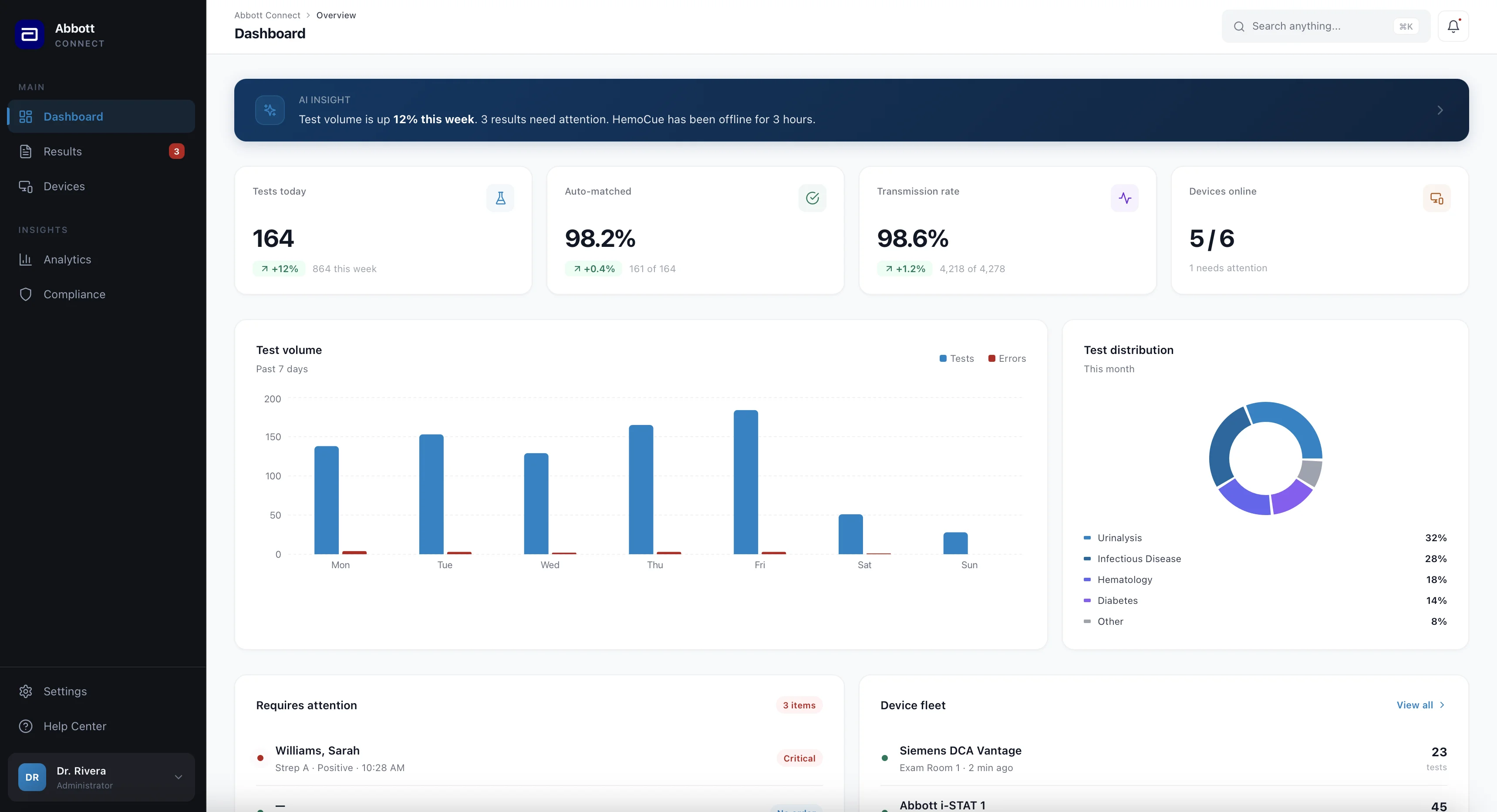
The Complete Platform
The ambient intelligence approach became the foundation, but the final platform synthesizes all three directions: alert-driven prioritization from Direction 3, data density from Direction 2, and structured device views from Direction 1. The result is 8 integrated views, from ambient dashboard to CLIA automation.
Explore the interactive prototype by navigating between Dashboard, Results, Devices, Analytics, and more
What I shipped
8-view prototype with WCAG AA design system, real data models, and working interactions.
RALS, AegisPOC, and RelayMed comparison with positioning map, personas, and battlecard.
Device-to-dashboard pipeline, onboarding wizard flow, QC validation, and failure recovery paths.
Strengths, vulnerabilities, win/loss scenarios, and objection handling for sales.
What I owned vs. supported
What this unlocks
What I took away
This concept work taught me that in healthcare, the hardest design problem isn't the interface. It's earning trust. Every clinician I spoke with had been burned by systems that promised automation and delivered complexity. That shaped every decision I made: the ambient alert model that stays quiet until something actually needs attention, the six-step wizard that proves the system works before asking for commitment, the compliance layer that turns a regulatory burden into a feature. When you're designing for people who can't afford downtime, clarity isn't a nice-to-have. It's the product.